By Nicola Perrin
Personal data is a sensitive subject at the best of times. Confidence in its safety and security is paramount. This chapter uses care.data as a case study to show what can happen without attitudinal insight and open and ongoing two-way dialogue to change public perceptions.
You’ll learn:
• Using patient data could help save lives, but patients must have confidence that their privacy is protected
• The failure of the care.data programme demonstrates how essential it is to communicate effectively with the public and healthcare professionals
• The NHS must lead a full conversation to explain how and why data can be used for care and research and how personal information is kept safe
Learning from care.data
In January 2014, every household in England was sent a leaflet, ‘Better information means better care’. The aim was to collect patient-level data from GP practices and to link this data with information from hospitals, registries and prescribing databases in order to provide better care, inform commissioning and advance research. The leaflet set out how information would be used and the choices people had.
Sounds good? Within a month, the care.data programme was put on hold, following a backlash in the media. It was finally abandoned two years later.
The project failed for two main reasons: the governance processes were found to be flawed and the communication strategy was extremely poor. The opportunity to make better use of patient data to improve health, care and services across the NHS has still not been realised.
Data saves lives
The NHS has a unique resource: patient records for nearly 60 million people, with information about the health of a very diverse population from cradle to grave.
If small amounts of data from many patients are linked up and pooled, researchers and doctors can look for patterns in the data, helping them develop new ways of predicting or diagnosing illness. The information from patient records is invaluable to help develop new treatments, monitor safety, plan NHS services and evaluate policies.
For example, researchers have been able to explore why diabetes rates vary between ethnic groups, demonstrate that bowel cancer screening is effective, check the safety of hip replacements and improve the delivery of kidney dialysis services.
Given the huge pressures facing the NHS, making more effective use of data is crucial to provide the best patient care and to make more effective use of scarce NHS resource.
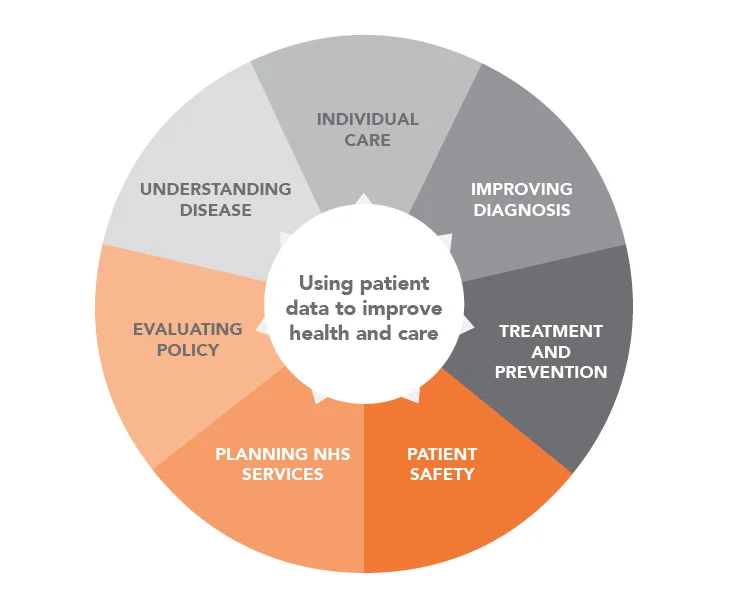
FIGURE 01 Using patient data to improve health and care
But patient data is sensitive and confidential. The NHS will only be able to realise the potential if everyone has confidence that data is kept safe and secure, with access appropriately controlled.
Currently, most people – whether the public, patients or healthcare professionals – know very little about how data is used which makes them wary.
Raising awareness
Public attitudes work suggests that more than two thirds of the population feel they do not know how health data is used in the NHS.
However, the evidence also shows that the more information people have, the more comfortable they are with wider uses of data. The results are fairly consistent: people are generally supportive of the use of data for research, provided there is a clear public benefit.
There is a caveat: giving only a small amount of information may actually raise concerns. Where people have questions over how data is used, giving too little information leaves them with unanswered questions. It is only by providing further information, about the benefits and the safeguards, that people become more reassured.
That is why it is so important that we get better at talking about patient data and why the National Data Guardian has called for a ‘fuller dialogue’ with the public.
In response, the Understanding Patient Data [1] initiative has been set up to support better conversations about the uses of health information. Our aim is to explain how and why data can be used for care and research, what’s allowed and what’s not and how personal information is kept safe.
Supporting better conversations
The first priority is to talk about the ‘why’, to explain the benefits of using data. For example, the #datasaveslives campaign has been successful in highlighting the positive impacts of analysing data.
But the failure of care.data also shows how essential it is to explain more about the safeguards and to be honest about any potential risks. There needs to be more transparency: everyone should be able to find out about how data is used, why and by who.
The provision of clear communication material will become even more important in 2018. The new data protection legislation, which must be implemented in May, has an increasing focus on fair processing. And the introduction of a new single national opt-out, as recommended by the National Data Guardian, will only be successful if there is a robust comms strategy clearly explaining the choices that people have so they can make an informed decision.
Engagement with healthcare professionals will be crucial to help achieve this. Doctors and nurses are the gateway to the public.
The Wellcome Monitor found that doctors, nurses and other medical practitioners emerge as the most trusted (64%) source of information about medical research, both because they are the experts and there is no reason to doubt them. [2]
Engaging the NHS workforce must be a key priority to ensure they have the resources to explain to their patients how data is used and to help implement the changes.
New digital technologies
A single conversation will not be enough. As the NHS turns 70, data-driven technologies are advancing rapidly. Machine learning algorithms can already differentiate between cancerous and healthy tissue more accurately – and more quickly – than the human eye. There is significant potential for artificial intelligence to transform healthcare and to help ensure a more sustainable NHS.
But there is also the risk of a public backlash if technology firms are seen to be processing vast quantities of data, in unexplained ways, at the expense of privacy. There must be meaningful public dialogue to help people understand the risks and benefits and to ensure that everyone can have confidence that data is being used in a responsible way.
Unlocking patient data will help improve health and care for us all. Data really can save lives. But if we are to achieve real improvements, patients, the public and healthcare professionals must have confidence that access to patient data is appropriately managed.
Part of demonstrating a trustworthy system is to provide clear, accessible and accurate information. We must learn from the mistakes of care.data to ensure effective communication. Together, we can champion responsible uses of patient data.
Sources
[1] https://understandingpatientdata.org.uk/
[2] Ipsos MORI (2016) Wellcome Trust Monitor, Wave 3. London: Wellcome Trust https://wellcome.ac.uk/sites/default/files/trust-in-medical-research-graphic-wellcome-apr16.pdf
Nicola Perrin leads the Understanding Patient Data initiative, focusing on supporting better conversations about uses of health information. Previously Head of Policy at the Wellcome Trust from 2007-2016, she was responsible for leading Wellcome’s policy development and advocacy work, with a particular focus on research base funding, data sharing and innovation in the NHS. Before joining Wellcome, Nicola worked at the Nuffield Council on Bioethics and at the Science Museum. She is a Trustee of the Association of Medical Research Charities and was included in the list of 50 Movers and Shakers in BioBusiness in 2017.
Twitter: @NMRPerrin
Online: www.understandingpatientdata.org.uk